Shared knowledge – infant mortality rate halved


Knowledge exchange between nurses and doctors in Norway and India has contributed towards improvements in nutrition, hygiene and increased participation by parents at two intensive neonatal care units in New Delhi.
As a result, infant mortality at the two units fell by close to 50 percent over the space of three years.
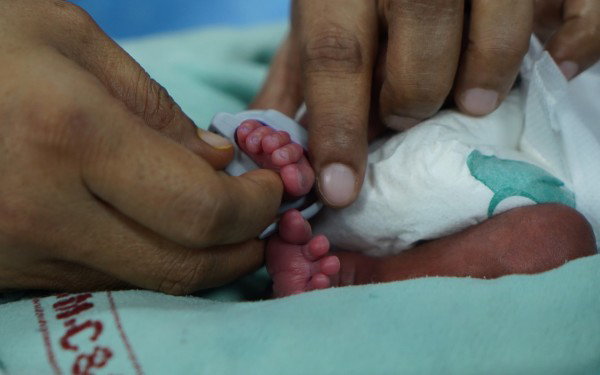
India is one of the countries worldwide with the highest rate of low birth weight in newborns. This is attributed to the high proportion of premature births, often combined with insufficient nutrition for the mothers while they are pregnant.
“India is a low-income country. The number of babies who require treatment and care is higher in India than in many other countries. At the same time, the infrastructure is insufficient, and we do not have good enough equipment and personnel,” explains project coordinator and doctor at Lady Hardinge Medical College & Kalawati Saran’s Hospital, Sushma Nangia.
Between one fourth and one half of deaths in newborn babies occur during their first week of life. For sick babies, good hygiene, breast milk and skin-to-skin contact with the mother and father can make the difference between life and death.

Long-term collaboration
Since 2012, the Division of Global Health at Oslo University Hospital (OUS) has taken part on a collaborative project with public hospitals in India. This exchange project has been financed by the Norwegian Agency for Exchange Cooperation (Norec).
The main objective for the project has been to improve treatment for unwell and premature babies in New Delhi, and to provide Norwegian health personnel with experience in diagnoses and treatment in relation to challenges not encountered in Norway. The project also has a clear objective to increase multicultural understanding within treatment of new-born babies.
Nurses from Ullevål Hospital spend 12 months on exchange at an Indian hospital, while nurses from India spend six months on exchange in Norway.
Changed the way they work
Shalini Rawat is a nurse at Lady Hardinge Medical College & Kalawati Saran’s Hospital, and spent six months on exchange, from October 2019 to March 2020, at Oslo University Hospital, Ullevål. She explains that the exchange has resulted in major changes at her workplace in Delhi.
“Before the exchange, we did things differently. We have learned so much from the exchange. We have changed the way we do things,” says Shalini Rawat.
In particular, there is one lesson she and her nursing colleagues have learned from their time in Norway, and that is a whole new approach.
“Norwegian nurses always go all in when they do something, no matter how minor or major the task. They are very dedicated. We have learned from this, and now we approach all our tasks with the same level of dedication,” explains Shalini Rawat.
Major benefits of breast milk
In 2017, a milk bank and breastfeeding centre were established at Lady Hardinge Medical College & Kalawati Saran’s Hospital in New Delhi, helping reduce infant mortality.
A milk bank is a service for mothers who, for different reasons, do not have enough breast milk to provide their babies with the best start in life. The World Health Organization (WHO) recommends breast milk from birth up to an age of six months.
The collaboration project has resulted in an increase in the number of babies who are either breastfed or receive expressed breast milk from 50 percent to close to 100 percent at the hospital units in India that have been involved in the project.
Ingvild Andresen, project coordinator at the Division for Global Health at OUS, explains that the use of breast milk at the neonatal wards in Delhi has more than doubled when compared to the period before the milk bank was set up. At the same time, the use of breast milk substitutes in Delhi has been halved two times.
“This is because mothers receive guidance on how to start breastfeeding, and because donor milk is provided instead of a breast milk substitute to the youngest babies before the mothers have been able to start breastfeeding,” explains Ingvild Andresen.
Before the exchange, we did things differently. We have learned so much from the exchange. We have changed the way we do things.

Continuous process
Project coordinator and doctor Sushma Nangia explains that a combination of many minor factors is behind the positive results achieved in the project.
“It is not possible to identify one sole factor that has resulted in the reduction in infant mortality. The nurses are more dedicated after the exchange. In combination with the milk bank, kangaroo care and amended routines (for example, hygiene routines), this has had wonderful results for our new-born babies. However, this is a total package that has been developed over time, and we are not done yet. We have to keep working on this,” says Sushma Nangia.
Indian nurses increased their level of dedication
Norwegian nurses refreshed "the clinical eye"
What do nurses do when they have to look after a sick child but do not have any technical aids? They use “the clinical eye.” Norwegian nurses on exchange in India had a small refresher in the use of the clinical eye.
“It’s easy to assume that Norwegian nurses won’t learn anything from working with health care in India. But that’s wrong,” says Ingvild Andresen.
She currently works as advanced nurse practitioner at the global section at Oslo University Hospital Ullevål, but she has previously spent time on exchange as a nurse in New Delhi.
She describes the exchange as a year full of impressions and learning.
“In Norway, we are surrounded by tons of equipment that we are used to having to help us determine a patient’s condition. In India, I had to refresh my clinical eye. Observing a child without access to the equipment we have in Norway made me more aware of my job,” she says.

Several light bulb moments
She travelled on exchange to Lady Hardinge Medical College & Kalawati Saran’s Hospital in New Delhi, from her position as an employee of Oslo University Hospital Ullevål, on a cooperation project financed by Norec.
Although the Norwegian participants were familiar with a milk bank and how it works, they had a few light bulb moments when they helped set up a milk bank and breastfeeding centre at the cooperating hospital in New Delhi.
“We wanted to use plastic bottles to feed the babies, because that is what we are used to in Norway. But we faced strong opposition,” says Ingvild Andresen.
The hospital where they were working prohibited the use of plastic bottles, basically because they were not able to clean the bottles properly.
“We learned that we had to use small steel bottles. This is a good example of how both parties contributed with our different types of know-how. And then we make use of what we can to achieve a good result, together,” she says.
Several of the Norwegian nurses on exchange were also able to improve their skills in both writing procedures and manuals.
“This is knowledge that we have brought with us back home and is very useful. We’ve also become more aware of our own culture thanks to the exchange. We arrived in India thinking that we were going to make some changes, but instead the changes were made to us. It’s good for us,” says Ingvild Andresen.
This is knowledge that we have brought with us back home and is very useful. We’ve also become more aware of our own culture thanks to the exchange. We arrived in India thinking that we were going to make some changes, but instead the changes were made to us. It’s good for us.

Cooperation reorganised due to COVID-19
When the COVID-19 pandemic broke out worldwide, it had an impact on the exchange project between the hospital in India and Oslo University Hospital Ullevål. The section for global health spent the spring of 2020 changing their project descriptions and reorganising their working methods.
“We have established a digital cooperation project to sustain our results after three years of cooperation,” says Kristin Schjølberg.
The focus groups meet once a month for both digital classes and seminars. This has allowed them to continue with mutual exchange of expertise, despite not being able to meet face to face. In addition, the groups proved their worth on a more human level when India was in the midst of the pandemic.
“The meetings were an arena for the nurses in New Delhi to debrief, and talk about their difficult experiences. During that period, the focus groups were just as much support groups and a safe place where nurses could debrief about their current situation,” says Kristin Schjølberg.